Dermatology
of interest
are looking at
saved
next event
Dermatology is the branch of medicine that specialises in the study of both normal and abnormal skin and its associated structures. Research and diagnosis of diseases, cancers, cosmetic and ageing conditions of the skin, fat, hair, nails, oral, and genital mucous membranes, are all aspects of dermatology. Healthcare professionals in this area regularly treat patients of all ages presenting with various inflammatory, inherited, environmental, occupational, or malignant skin disorders.
Learning Zones
EADV 2023: A new era for epidermolysis bullosa
An Industry Expert Hub session on 11 October 2023, hosted by Cristina Has, explores the latest research developments in and outside the clinic for epidermolysis bullosa. Watch highlights and expert interviews here.
To date, there are approximately 2000 distinct diseases affecting the skin with many variants. Although many skin diseases are harmless and asymptomatic, others are associated with significant disability, increased morbidity, and reduced quality of life.
The dermatologist is involved in the treatment and prevention of a wide range of skin disorders. They employ various investigations to diagnose and medicine-based or surgical interventions to treat various types of skin conditions. These include, but are not limited to, dermatopathology, dermatologic and cosmetic surgery, topical and systemic medicines, immunotherapy, and phototherapy. As well as seeing patients in dermatology clinics, dermatologists act as consultants to other clinical specialists or perform clinical or basic research.
This Dermatology Speciality Hub is an expert educational resource, intended for healthcare professionals, that provides credible medical information in the form of Learning Zones. These Learning Zones provide self-directed medical education about common skin disorders such as skin cancer, urticaria, various types of psoriasis, and atopic dermatitis.
In this section
Alopecia areata
Containing relevant Learning Zones, guidelines, trials and news.
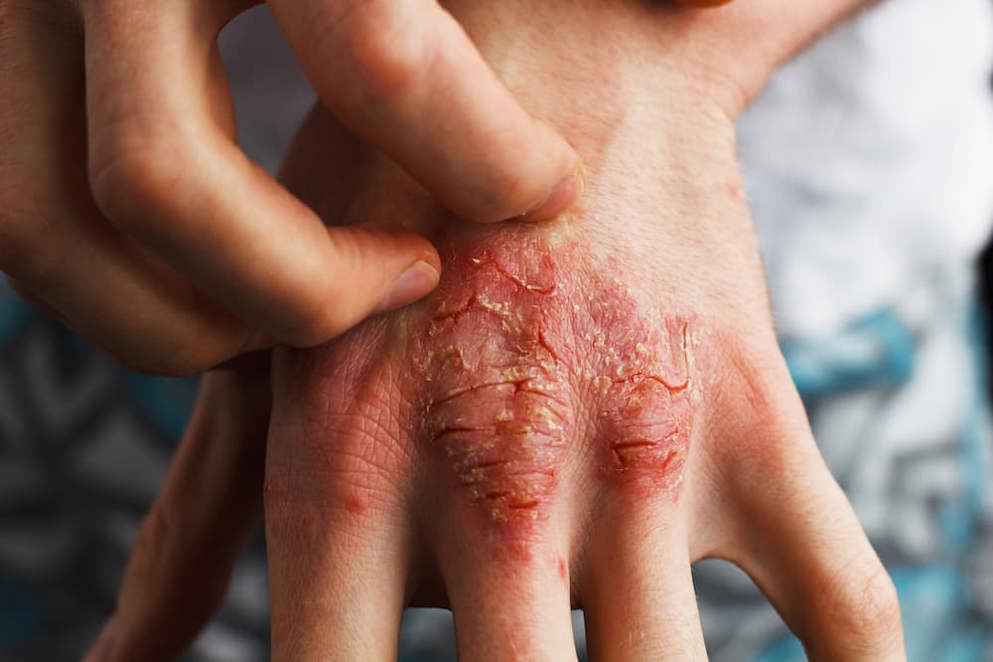
Atopic Dermatitis
Containing relevant Learning Zones, guidelines, trials and news.
Hidradenitis suppurativa
Containing relevant Learning Zones, guidelines, trials and news.
Herpes Zoster
Containing relevant Learning Zones, guidelines, trials and news.
Psoriasis
Containing relevant Learning Zones, guidelines, trials and news.
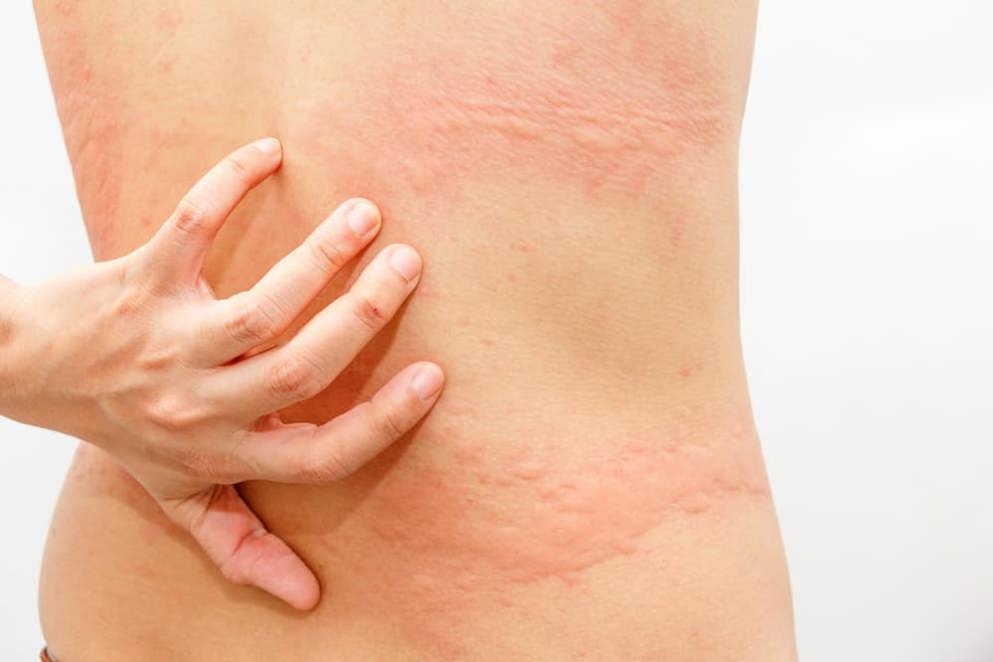
Urticaria
Containing relevant Learning Zones, guidelines, trials and news.