Welcome
How much do you know about inflammatory bowel disease (IBD)?
- Gain insights into the pathophysiology of Crohn’s disease and ulcerative colitis
- Understand the risk factors and symptoms associated with IBD
- Discover more about available treatment options, including advanced therapies
- Familiarise yourself with international guideline recommendations
Explore our dedicated Learning Zone to find out more about Crohn’s disease and ulcerative colitis, including the epidemiology and immunology of these complex and debilitating diseases. You will also find information on recently approved treatments for patients with IBD and much more.
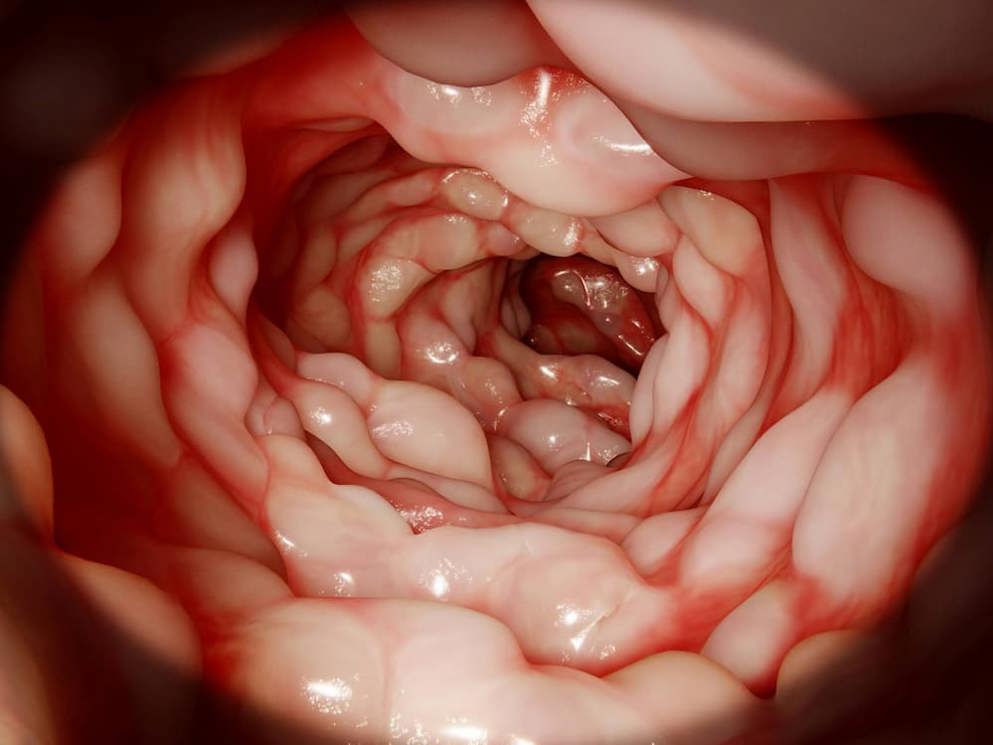
Understanding Crohn’s disease
What is Crohn’s disease and how does it affect patients?
Understanding ulcerative colitis
What is ulcerative colitis and how does it affect patients?
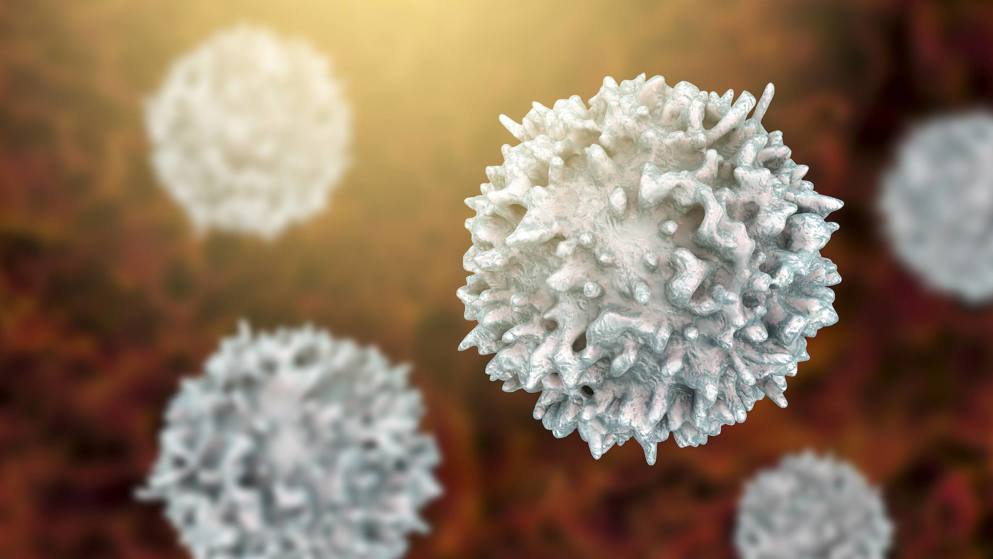
Immunology of IBD
Learn more about immune response dysregulation in IBD.
Treating IBD
Understand IBD treatment options and how treatment goals are evolving.
of interest
are looking at
saved
next event
Developed by EPG Health for Medthority in collaboration with Takeda, with some content provided by Takeda.
C-ANPROM/INT/IBDD/0041 October 2021.